Pouch of Douglas: Anatomy, Fluid Causes & Fertility Impact
The pouch of Douglas is more than a medical term—it’s a diagnostic window into pelvic health that every woman should understand. This small anatomical space behind the uterus collects fluid that can reveal everything from normal menstrual changes to serious conditions like endometriosis, making it a critical indicator when fertility is at stake.
Location: Between uterus and rectum · Also called: Rectouterine pouch, cul-de-sac · Found in: Females only · Common issue: Free fluid accumulation · Associated conditions: Endometriosis, ovarian cysts
Quick snapshot
- The pouch of Douglas is the lowest peritoneal point in a standing woman, making it a gravity-fed collecting space for fluid (Your Health Magazine)
- It is present in all females and is named after James Douglas, the Scottish anatomist who first described it (Your Health Magazine)
- Researchers have not established a definitive clinical threshold for what counts as an “abnormal” amount of fluid in the pouch (Voluson Club clinical ultrasound resource)
- Whether fluid accumulation directly causes infertility or merely signals underlying pathology remains contested (Voluson Club clinical ultrasound resource)
- Fluid volume fluctuates with the menstrual cycle: roughly 5 ml in the early follicular phase, climbing to around 20 ml during the early and midluteal phases (Voluson Club clinical ultrasound resource)
- Ovulation and menstruation are the two moments when cul-de-sac fluid collection peaks (Voluson Club clinical ultrasound resource)
- Transvaginal ultrasound is the primary tool for visualizing pouch of Douglas fluid during routine gynecological assessment
- When fluid is accompanied by pain or infertility, further investigation for endometriosis or ovarian pathology typically follows
A quick-reference table puts the core facts in one place:
| Label | Value |
|---|---|
| Scientific name | Rectouterine pouch |
| Named after | James Douglas |
| Depth | Lowest peritoneal point in the pelvis |
| Gender specific | Females |
| Normal fluid baseline | 1–3 ml (4–5 ml during ovulation) |
| Cul-de-sac fluid in endometriosis | 80.5% prevalence on ultrasound |
What Is the Pouch of Douglas?
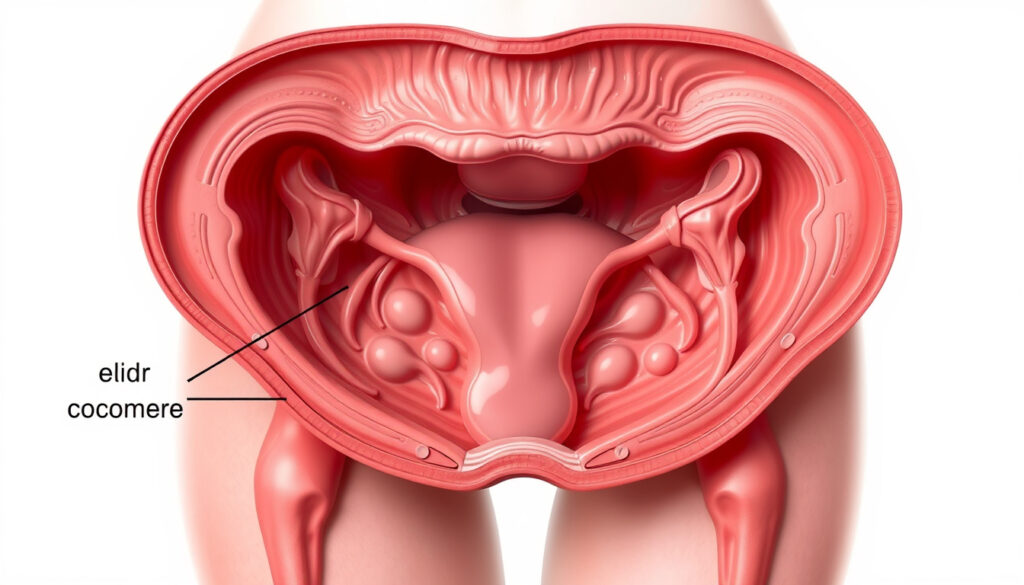
The pouch of Douglas—also called the rectouterine pouch or, more colloquially, the cul-de-sac—is a peritoneal pocket situated between the back wall of the uterus and the front surface of the rectum. It represents the deepest point of the abdominopelvic cavity in a person standing upright, which means gravity causes any loose fluid in the pelvis to pool there naturally.
This anatomical feature exists in all females from birth. It owes its name to James Douglas, the 18th-century Scottish anatomist who provided one of the earliest detailed descriptions of the region. While the pouch itself has no known hormonal function, it serves as a sensitive indicator of what’s happening in the surrounding pelvic structures—making it clinically significant when something goes wrong.
Location and anatomy
The pouch of Douglas sits behind the uterus, separated from the rectum only by a thin peritoneal membrane. Its proximity to both reproductive and gastrointestinal organs means it can collect fluid from multiple sources: menstrual blood that refluxes backward through the fallopian tubes, blood from a ruptured ovarian cyst, or inflammatory exudate from an infection in the pelvis.
Two pelvic cul-de-sacs exist in total. The posterior cul-de-sac (the pouch of Douglas) is the one most frequently discussed in clinical contexts because it sits at the gravity-dependent point of the peritoneal cavity, making it the primary site for fluid accumulation both in health and disease. The anterior cul-de-sac, by contrast, lies between the bladder and the uterus—a less relevant space for fluid pooling.
Alternative names
The pouch of Douglas is most commonly referred to by its eponym, though “rectouterine pouch” is the more formal anatomical term. In clinical and radiology literature, “cul-de-sac” appears frequently, borrowed from the French for “bottom of the bag.” Some physicians also use “posterior cul-de-sac” to distinguish it from its anterior counterpart.
Because the pouch of Douglas collects everything that pools at the bottom of the pelvis, it acts as a diagnostic window—fluid visible here on an ultrasound is often the first clue that something abnormal is occurring in the upper pelvic cavity.
What causes a pouch of Douglas fluid?
Not all fluid in the pouch of Douglas signals disease. The space normally contains a small amount of peritoneal fluid that fluctuates across the menstrual cycle. Research published in the Archives of Perinatal Medicine suggests a baseline range of 1 to 3 ml under normal circumstances, with 4 to 5 ml considered typical during ovulation when hormonal changes increase peritoneal secretion.
During the early follicular phase, peritoneal fluid in the posterior cul-de-sac measures roughly 5 ml on average. That figure climbs to about 20 ml in the early and midluteal phases, according to data from Voluson Club, a clinical resource for ultrasound practitioners. These cyclic variations are physiological and expected—a woman may notice more fluid on imaging during days 14–20 of her cycle than during the first week.
Normal versus abnormal fluid
The challenge for clinicians is that no universally accepted threshold distinguishes “normal” from “abnormal” pouch of Douglas fluid. A small amount of fluid is expected; a large amount may indicate pathology—but where that line sits varies from patient to patient and depends heavily on clinical context. Ultrasound practitioners assess fluid volume alongside the patient’s symptoms, menstrual cycle timing, and other imaging findings.
Certain patterns do raise red flags. Echogenic fluid—fluid that appears bright or clotted on ultrasound—may signal a ruptured ectopic pregnancy or hemorrhagic ovarian cyst, according to Voluson Club’s analysis of transvaginal imaging findings. Low-level echo hemoperitoneum can indicate that a hemorrhagic cyst has recently ruptured, releasing blood into the peritoneal cavity.
Common medical causes
When fluid accumulation exceeds what the menstrual cycle would explain, several conditions are typically responsible:
- Ovarian cyst rupture: A functional cyst that bursts can spill fluid and blood into the pouch of Douglas. This is often self-limiting but may cause acute pain.
- Endometriosis: Endometrial tissue implanted outside the uterus—particularly in the posterior cul-de-sac—produces inflammatory fluid and can cause adhesions that trap organs together. Research from PubMed (a study of 182 consecutive infertility patients) found the posterior cul-de-sac involved in 34% of endometriosis cases, while the uterosacral ligament was affected in 28%.
- Pelvic inflammatory disease (PID): Infections of the upper reproductive tract cause inflammatory exudate that pools in the pouch of Douglas. Untreated PID can lead to scarring and fallopian tube damage.
- Ectopic pregnancy: A pregnancy implanted outside the uterus, typically in the fallopian tube, can cause bleeding into the peritoneal cavity when it ruptures. This represents a medical emergency.
Free fluid in the pouch of Douglas doesn’t directly cause infertility—but it frequently signals conditions (endometriosis, PID) that do. The fluid is often a symptom, not the underlying problem.
What is free fluid in the pelvis?
Free fluid refers to any liquid that exists unbound in the peritoneal cavity, as opposed to fluid contained within an organ or cyst. When a radiologist or sonographer reports “free fluid in the pelvis,” they are describing fluid that has escaped into the abdominal cavity and accumulated at its lowest gravitational point—the pouch of Douglas.
Because the two pelvic cul-de-sacs are the most dependent spaces in the pelvis (whether a patient is upright or lying flat), fluid from any source above them will eventually collect there. This makes the pouch of Douglas the first place clinicians look when they suspect intra-abdominal bleeding, infection, or peritoneal irritation.
Detection on ultrasound
Transvaginal ultrasound is the preferred imaging modality for visualizing pouch of Douglas fluid. The probe sits close to the pelvic organs, providing high-resolution images of structures that abdominal ultrasound struggles to penetrate.
Any significant cul-de-sac fluid should be easily visible on transvaginal ultrasound, which is why the test is routinely used in the workup of pelvic pain, suspected ovarian pathology, and infertility evaluation. The appearance of the fluid—clear versus echogenic, minimal versus moderate volume—provides clues about its origin and urgency.
Clinical significance
Free fluid in the pelvis ranges from entirely benign to life-threatening. A small amount in a premenopausal woman scanned mid-cycle may require no action at all; the same finding in a woman with acute lower abdominal pain and a positive pregnancy test demands immediate investigation for ectopic pregnancy.
The clinical context determines urgency. Ultrasound findings are interpreted alongside the patient’s history, symptom onset, and laboratory results—not in isolation. A radiologist’s report of “free fluid in the posterior cul-de-sac” is just one piece of a larger puzzle.
Can I get pregnant with pouch of Douglas?
The presence of fluid in the pouch of Douglas does not automatically prevent pregnancy, but it can complicate the path to conception in several ways. The relationship between pouch of Douglas fluid and fertility is indirect but clinically meaningful.
Conditions that produce abnormal fluid—most notably endometriosis and pelvic inflammatory disease—also cause structural damage to the reproductive system. Scarring and adhesions in the fallopian tubes, impaired ovum pickup by the fimbriae, and altered peritoneal environment all reduce the odds of successful fertilization and implantation.
Link to infertility
Research from Mamata Fertility (a fertility treatment center) explains that accumulated fluid may affect sperm motility by creating an unfavorable chemical environment in the peritoneal cavity. Sperm incubated in the free fluid of patients with endometriosis suffered significantly greater DNA damage compared with sperm that swam in the fluid of women without the condition, according to findings discussed in clinical literature.
The same study also noted reduced sperm motility and fewer progressively motile sperm in the presence of cul-de-sac fluid from endometriosis patients. This suggests the fluid itself—not just the underlying condition—may play a role in degrading male reproductive cells.
Additionally, the presence of fluid can impair the uterus’s ability to support embryo implantation. When the peritoneal environment is altered by inflammation, the endometrium may become less receptive to an implanting embryo, limiting the chances of a successful pregnancy.
Endometriosis role
Endometriosis is the condition most tightly linked to pouch of Douglas pathology and infertility. The disease causes endometrial-like tissue to implant on surfaces including the posterior cul-de-sac, uterosacral ligaments, and ovaries. These implants respond to hormonal cycles, bleed internally, and trigger inflammation that leads to adhesion formation.
In a laparoscopic study published on PubMed involving 182 consecutive patients with infertility and endometriosis, the ovary was the most common site of endometrial implants, with 54.9% showing unilateral or bilateral involvement. The posterior broad ligament ranked second at 35.2%, followed by the anterior cul-de-sac (34.6%), the posterior cul-de-sac (34.0%), and the uterosacral ligament (28.0%).
Adhesion formation follows the same anatomic distribution as the endometrial implants themselves—a critical finding because adhesions can physically restrict the movement of the ovaries, fallopian tubes, and uterus, impairing egg release, sperm transport, and embryo implantation.
When the pouch of Douglas is covered by adhesions, the chance of natural pregnancy is lower, according to guidance from Endometriosis UK. In severe cases, the pouch becomes partially or completely obliterated—the organs fuse together due to scar tissue, eliminating the normal sliding movement between them.
The sliding sign, a dynamic transvaginal ultrasound test, can diagnose pouch of Douglas obliteration preoperatively, according to research published in PMC/NIH. This allows surgeons to plan more effectively for the complex surgery required to restore pelvic anatomy.
For women trying to conceive, addressing endometriosis—through laparoscopic surgery, hormonal suppression, or assisted reproductive technology—offers the most realistic path to pregnancy when pouch of Douglas involvement is present.
What are the symptoms of Douglas pouch issues?
When the pouch of Douglas is involved in a pathological process, symptoms vary depending on the underlying cause. Some women experience significant disease in this region with minimal symptoms; others have pronounced pain from relatively minor findings.
Pain and digestive issues
Pelvic pain is the most common complaint associated with pouch of Douglas pathology. Endometriosis implants in the posterior cul-de-sac can cause deep dysmenorrhea (painful periods), chronic pelvic pain, and dyspareunia (painful intercourse). Because the region sits adjacent to the rectum, bowel symptoms are also common: painful bowel movements, constipation, and pain during defecation.
Patients with endometriosis affecting the pouch of Douglas can suffer from a combination of gynecological and gastrointestinal symptoms, according to Endometriosis Australia. Bloating, changes in bowel habit, and rectal bleeding (if implants invade the bowel wall) may accompany menstrual pain.
When an ovarian cyst ruptures and spills fluid into the pouch of Douglas, the pain is often sudden and sharp. Some women describe it as feeling like something “popped” inside them. The pain may localize to one side of the pelvis and can radiate to the lower back or thigh.
When to seek help
Certain signs warrant urgent evaluation: sudden severe pelvic pain, pain accompanied by fever or vomiting, fainting or lightheadedness, or pain after a missed period with a positive pregnancy test. These may indicate ectopic pregnancy, ovarian torsion, or severe internal bleeding.
For chronic symptoms—recurring pelvic pain, pain during intercourse, or difficulty conceiving after 12 months of unprotected intercourse—a gynecologist or reproductive specialist can perform the imaging and laboratory work needed to identify the underlying cause and guide treatment.
Cul-de-sac endometriosis is difficult to diagnose on physical exam alone. Transvaginal ultrasound can identify fluid accumulation, endometriomas, and adhesions—giving women a clearer picture of what’s affecting their fertility before they invest in treatment plans.
Quotes
“The pouch of Douglas collects menstrual blood refluxed through the fallopian tubes, along with any hemoperitoneum from ruptured ovarian cysts.”
— Voluson Club clinical ultrasound resource
“The two pelvic cul-de-sacs are the most dependent spaces in the pelvis when a patient is either upright or supine.”
— Voluson Club clinical ultrasound resource
“If the pouch of Douglas is covered by adhesions, the chance of getting pregnant is lower.”
— Endometriosis UK patient guidance organization
Bottom line
The pouch of Douglas is a small space with major clinical significance. It naturally collects fluid from across the pelvis, making it a useful diagnostic window for conditions ranging from normal menstrual cycle changes to ectopic pregnancy, ovarian cyst rupture, and endometriosis.
For women experiencing pelvic pain or struggling to conceive, fluid visible in the pouch of Douglas on an ultrasound is worth investigating—not because the fluid itself is the problem, but because it often signals something that is. Endometriosis and pelvic inflammatory disease are the most common culprits, and both are treatable.
For women trying to get pregnant, the takeaway is that pouch of Douglas fluid is a clue, not a sentence. Working with a gynecologist or reproductive specialist to identify the underlying cause—rather than focusing on the fluid itself—offers the best path forward.
Related reading: Can Fluid in Pouch of Douglas Cause Infertility? Causes & Treatment · Exploring the Pouch of Douglas: Importance and Health Implications
endometriosis-uk.org, pubmed.ncbi.nlm.nih.gov, drseckin.com, endometriosisaustralia.org, youtube.com
Frequently asked questions
What is the pouch of Douglas for?
The pouch of Douglas has no known physiological function. It is simply the deepest point of the peritoneal cavity in a standing woman, meaning fluid naturally collects there. Its clinical importance lies in what it reveals: when abnormal fluid pools here, it often signals pathology elsewhere in the pelvis.
Do females have pouch of Douglas?
Yes. The pouch of Douglas is present in all females from birth. It is a peritoneal space between the uterus and rectum. Males do not have a pouch of Douglas because they lack a uterus—the anatomical structures that define the space simply do not exist in the male pelvis.
Do C-sections leave you with a pouch?
No. The pouch of Douglas is a normal anatomical feature that exists regardless of surgical history. A Caesarean section does not create, remove, or alter the pouch of Douglas. The misconception may arise from confusion about adhesions—scar tissue from prior pelvic or abdominal surgery can sometimes involve the region, but this is not specific to C-section.
What are red flags for ovarian cysts?
Red flags include sudden severe pelvic pain, pain accompanied by fever, vomiting, or fainting, and pain in early pregnancy. Large cysts (over 5–7 cm), complex cysts with solid components, and cysts that grow rapidly also warrant urgent investigation. Rupture or torsion are surgical emergencies.
What cancers can spread to the peritoneum?
Several cancers can metastasize to the peritoneum, including ovarian cancer, colorectal cancer, gastric cancer, and pancreatic cancer. When peritoneal metastases involve the pouch of Douglas region, fluid accumulation may occur. This finding on ultrasound or CT scan often indicates advanced disease and influences treatment planning.
How to tell if you’re extremely fertile?
There is no reliable way to self-assess fertility without medical testing. Signs such as regular menstrual cycles, ovulatory discharge, and absence of pelvic pain are suggestive but not conclusive. A fertility evaluation with a reproductive specialist includes hormone testing, ultrasound imaging, and potentially a hysterosalpingogram to assess tubal patency.
Pouch of Douglas also known as?
The pouch of Douglas is also called the rectouterine pouch, posterior cul-de-sac, or simply the cul-de-sac. In anatomy textbooks, “rectouterine pouch” is the preferred formal term.